
| Vol.
XXX No.
4 March / April 2018 |
| contents |
| Printable Version |
Improving the Urgent Care Experience
Through Student-Informed Care
Like all departments, labs, and centers, MIT Medical is always looking for ways to evolve and improve. Whether it’s focusing closer on the customer experience, being more fiscally responsible, or turning our attention toward planning for the future, we are constantly striving to be our best.
In that spirit, in 2016, MIT Medical commissioned a patient journey map that used data-driven methodology to give us a holistic view of how our patients experience care at MIT Medical. This involved analyzing more than 1,000 comments from post-visit surveys, interviewing staff, and shadowing patients. In the end, our journey map (see below) identifies every touchpoint within an episode of care and highlights touchpoints where we’re exceeding patient expectations as well as opportunities for improvement.
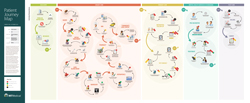
(click on image to enlarge)
The map tracks the experiences of a fictional patient, “Josh Junior,” who sustains an injury while playing flag football. Our use of a student persona for this mapping exercise was deliberate. After all, students are at the core of the Institute’s mission and are, by extension, the very reason for MIT Medical’s existence.
Josh’s journey begins with his impressions of MIT Medical before becoming a patient and follows him through his initial visit to Urgent Care and subsequent need for specialty and primary care.
From the start, we knew that a student-focused map would put a particular spotlight on our Urgent Care service. For most MIT students, Urgent Care is their first exposure to MIT Medical; for many, it is the only interaction they have with MIT Medical during their time in Cambridge. Our 18,000 Urgent Care visits each year account for approximately 15 percent of clinical encounters across all of MIT Medical. Not surprisingly, students account for 58 percent of Urgent Care visits.
Gathering More Data
Following our internal operational analysis, we were fortunate to work with a talented team of four students enrolled in Sloan’s Health Systems Innovation Healthcare Lab (H-Lab) course. As part of the requirements for this course, students undertake a four-month-long action learning project in host healthcare institutions. These projects typically involve looking at complex problems in Internet technologies, operations management, strategic marketing, and other areas. Similarly to the journey mapping process, our H-Lab team collected and analyzed data, interviewed stakeholders, and synthesized a set of concerns:
- Reputation: We have a reputation problem with students. Our wait times are not transparent, and they can be long, sometimes up to four hours. Students also have concerns about privacy during check-in and triage.
- Systems and operations: Our systems and operating processes are unaligned, inefficient, and sometimes fall short of meeting patient expectations. This includes everything from staffing and the check-in process, to our hours of operation and the ways clinical staff communicate with each other.
- Identity: Urgent Care has an identity crisis. Is it an emergency room? (Answer: No) Is it primary care? (Answer: No) Is it convenient care? (Answer: Well, the location is convenient, but the long wait times aren’t.) To further confuse the issue, unlike many local urgent care facilities, ours doesn’t offer ancillary services like lab or radiology after hours or on weekends.
The result of all of these issues is a disjointed patient experience that disproportionally affects students.
Putting Patients First
As part of this process, we have also turned to our internal experts for their advice. For example, within the field of mental health, there is a well-known best-practice model known as trauma-informed care. This means building a practice that is a safe space for trauma survivors – where they feel safe, understood, and listened to. Trauma-informed care can take many forms, from redesigning intake forms to replacing bench-like seating in waiting areas with individual seats that don’t force trauma survivors to sit in close proximity to strangers. But at its heart, trauma-informed care means placing the care of one’s most vulnerable patients at the core of an organization’s mission and vision.
As mental health practices began to adopt this care model, they discovered something interesting – that the changes they made to become more sensitive to trauma survivors were also welcomed by patients who were not trauma survivors. That when you design a system to provide the best possible care to the most vulnerable patients, it improves care for everyone.
Everyday examples of this phenomenon can be found in the environment around us. Closed captioning, originally intended to benefit deaf and hard of hearing individuals, now allows everyone to access television programing in noisy bars, gyms, and airports. Similarly, access ramps and sidewalk curb cuts are utilized not only by wheelchair users, but by countless others – parents pushing strollers, delivery people with handcarts, travelers with rolling luggage, and many more.
With this model in mind, Associate Medical Director and Chief of Mental Health and Counseling Karen Singleton and Chief of Student Health Shawn Ferullo have suggested that the organizing principle for MIT Medical should be what they are calling student-informed care.
While MIT students are exceptionally intelligent and capable individuals, as patients, they remain our most vulnerable group. Many are novices at seeking healthcare independently, and few have established clinical relationships at MIT Medical. By restructuring our practice to provide the best possible care for students – our least savvy healthcare consumers and our most vulnerable patient population – we believe we can elevate the care we provide to all our patients.
| Back to top |
Urgent Care Reimagined
As our Urgent Care Service evolves to provide more student-informed care, let’s imagine how different Josh Junior’s next experience will be:
Early one Saturday morning, around 2 am, Josh starts to feel ill. He goes online to medical.mit.edu to see what to do. The website has information about common ailments and suggests that Josh’s symptoms are severe enough that he should call for advice. When Josh calls, he reaches a friendly nurse, who listens, is sympathetic, and instructs him to try to get some rest. She tells him that if he feels worse or the same in the morning, he should come in after 8 am, when Urgent Care opens.
Josh wakes up and still feels unwell. But though Josh is sick, his ailment is hardly urgent. He reaches for his phone and visits the MIT Medical website, where he sees that the current wait time in Urgent Care is 45 minutes. He doesn’t want to wait that long, and since it’s a Sunday with no classes, he uses the website to make an appointment for a few hours later, sets his alarm, and goes back to sleep.
Later, Josh makes his way to MIT Medical. By now, Urgent Care has most likely been renamed to better reflect the type of service we provide — MIT Medical Convenient Care, Same-day Care, or Walk-in Clinic. When Josh arrives, the signage is clear, and a friendly person at the front desk guides him to a check-in kiosk. After scanning his ID and answering some questions on a touch screen, he’s checked in – no more clipboards, paper forms, and pens, or having to discuss what is bothering him in a somewhat public setting. The system alerts us that he has arrived and tells us why he is here.
Josh takes a seat in the comfortable waiting area, where he finds snacks, a coffee machine, and charging station for his phone. Since he made an appointment earlier, a medical assistant greets him promptly. He is discreetly called to an exam room, where the medical assistant takes his vital signs and communicates that information to the doctor or nurse practitioner who will treat him. When the clinician comes into the room, he or she can begin treating Josh immediately. There will be no repetitive “What brings you in here today?” questions, because Josh has already provided that information and talked with the medical assistant.
Josh and his clinician look at his medical record together on the large flat-screen TV on one exam-room wall. The clinician gives Josh a prescription and instructs him to go to the lab to get some blood work done. Before he leaves, Josh is handed an iPad to fill out a quick survey about his experience.
Then he heads to the lab, which, along with the pharmacy, is conveniently open during the same hours as Urgent Care – even on weekends. He doesn’t have to leave campus to get his blood test or fill his prescription, so he can begin taking his medication right away. In under an hour, he’s back at his dorm, and when he feels better, he tells his friends about the great experience he had at MIT Medical.
Over the coming year, our team at MIT Medical will be working to make this vision a reality. Our new electronic medical record, patient portal, and practice-management system implementation in June 2018 will be a big step toward realizing these aspirations. After reviewing our data and conducting several pilots looking at our hours, we also anticipate changing the operating hours for Urgent Care to 8 am to 8 pm 7 days per week, likely with the next academic year. This change enables us to open lab, radiology, and pharmacy for expanded hours, thus improving our ability to care for our students and other patients during the times we are open. Additional work is also underway to evaluate the benefits of a new name and brand, and to improve staffing patterns, patient flow, and facilities.
Through data collection, listening, and our transformation to a student-informed care model, MIT Medical’s Urgent Care Service will deliver the best possible care to the MIT community. By focusing on student needs, we will elevate the experience of every patient who walks through our doors.
| Back to top | |
| Send your comments |
| home this issue archives editorial board contact us faculty website |